In the one week between June 28 and July 5, Bengaluru’s COVID-19 count more than tripled, with 7240 new cases. The surge in cases has overburdened the city’s healthcare capacity, and as a result, there have been many reports of patients not finding hospital beds or treatment on time. This has led to panic and confusion about what one should do on testing COVID-positive.
“The panic and fear of COVID is actually worse than COVID itself. That’s what we have to address before anything else,” says Dr Giridhara R Babu, Professor, Head-Lifecourse Epidemiology, Indian Institute of Public Health. Dr Giridhar is a member of the state government’s COVID expert committee as well as the ICMR task force for COVID.
In case you or a family member suspect COVID or test positive, what do you need to do? Here is a guide on how you can be prepared, and what measures you can take.
1. Prevention
“We were late in increasing capacity, but now most things are in place and all that’s left is community participation. The first thing for citizens to do is to protect themselves – avoid the 3Cs and do the 3Ws”, says Dr Giridhara.
Avoid the 3Cs:
- Closed spaces with poor ventilation
- Crowds (more than 2 people)
- Close Contact
Follow the 3Ws:
- Watch your distance (social distancing of at least six feet)
- Wear a Mask
- Wash your hands
2. What to do if you develop symptoms?
According to Dr Giridhara, in the majority of cases, patients develop only mild/moderate symptoms or no symptoms at all.
Common early symptoms are:
- Cough
- Fever
- Shortness of breath
- Sore throat
- Congestion
- Headaches
- Body Aches
- Sudden loss of smell and taste, commonly reported by new COVID patients.
However, some asymptomatic patients may not experience any of these.
Stay home: “If you develop symptoms, don’t panic. The important thing is to stay at home and isolate yourself,” says Dr Giridhara.
On July 4, state government initiated a policy of permitting home isolation for asymptomatic or mild patients, indicating they can be treated sufficiently well at home.
Keep a pulse oximeter handy: Blood oxygen saturation levels (SpO2) play an important role in determining the severity of symptoms. If the SpO2 level is below 90%, the patient’s condition is considered severe and they need urgent treatment. If the level is above 95%, the patient is considered mostly asymptomatic. “We are requesting the government to provide oximeters for every patient who is advised home isolation,” says Dr Giridhara.
Consult a doctor: If you notice symptoms, talk to a doctor, preferably through tele-consultation. You can also use the ArogyaSetu Self Assessment App. Based on this preliminary assessment, the decision on whether or not to get tested should be made.
Testing Criteria: All symptomatic patients from containment and buffer zones with ILI and SARI symptoms (acute respiratory infection with fever AND cough) will be tested immediately. Those from non-containment and buffer zones will be tested based on doctor’s advice.
Getting Tested: Until the results of tests are out, you should stay isolated at home as much as possible, according to Dr Giridhara.
Testing is done at fever clinics/swab collection centres at the district and taluk levels. There are at least 113 fever clinics/swab collection centres in Bengaluru (66 private and 47 government), where your samples can be taken.
From fever clinics/swab collection centres, samples are sent to one of the 25 ICMR-approved testing labs in Bengaluru. All fever clinics and labs send all test reports to the BBMP or the State Health Department. Hence, you may not get your results from the lab and may instead get them from BBMP.
Details of BBMP Health Officers
You can contact the Health Officer of your BBMP zone, in case of emergencies. They are also responsible for testing primary contacts of COVID-positive patients.
| East Zone | Dr Siddappa | 9480684214 |
| West | Dr Hegde | 9480683928 |
| South | Dr Shivakumar | 9480973395 |
| R.R. Nagar | Dr Balasundar | 9480685435 |
| Dasarahalli | Dr Balasundar | 9480685435 |
| Bommanahalli | Dr Suresh | 9480683473 |
| Yelahanka | Dr Savitha | 9480684570 |
| Mahadevapura | Dr Surendra | 9801750539 |
Quarantine Vs Isolation
- Quarantine: Restricting movement of people who may have been exposed to the virus, to check if they are developing any symptoms.
- Isolation: Separating the suspected and/or infected person from those who have not contracted the virus.
Source: Bengaluru Apartment Federation Guidelines
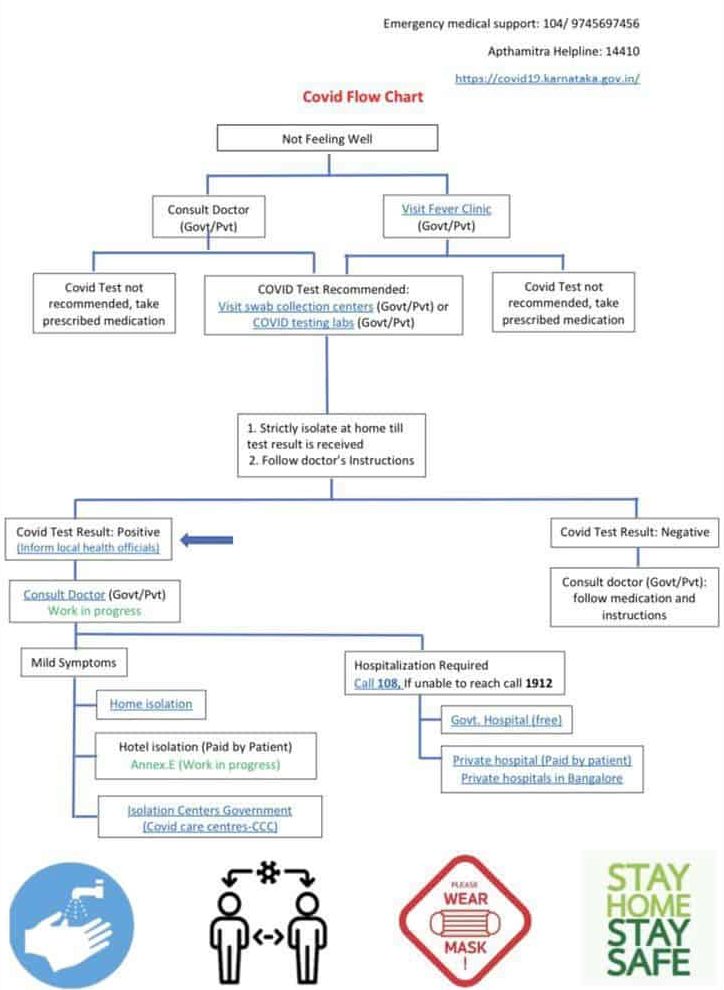
3. What if you test positive?
If you test positive, first inform your District Surveillance Officer (DSO)/BBMP local ward officials, and call one of the following helplines:
- 14410
- 104
- 080-1077
- 080-22967200
If you are an apartment resident, you should immediately inform your local residential/apartment association, who can offer support and ensure that authorities are informed.
Labs will directly inform the BBMP/State authorities about positive results. BBMP is to send a health team to the patient’s residence for a medical screening. They will check the patient’s body temperature, SpO2 levels and co-morbidities (like hypertension, diabetes, TB, HIV, cancer, etc.)/pregnancy.
Depending on your symptoms, the health team will decide if you are eligible for home isolation or need treatment at a COVID facility.
Preparing an Isolation Kit
Whether you are eligible for home isolation, or if you need to go to a care centre or hospital, it is good to get a kit ready. (Courtesy: Design Beku)
| Information 1) Contacts of family doctor/neighbourhood doctor, RWA office bearers/local volunteers 2) Contact numbers of COVID helpline of your district, district hospital, ambulance, medical store, medical oxygen cylinder provider, local plasma bank, people who have recovered recently from COVID-19, private and government COVID-19 testing labs servicing your area. Documents 1) Insurance details, medical records, list of allergies, etc. 2) Form for COVID testing: Spare copies with data filled for everybody, to save on exertion when you are sick 3) Home isolation declaration, printed, with a few spare copies and extra blank sheet | Other Items 1) Finger pulse oximeter with spare batteries. Epidemiologist Rifa Khan suggests procuring one per family, or the local RWA or apartment association could keep a few stocked. 2) Face masks, thermometers, regular medicines 3) Toiletry and sanitation kit 4) Water bottle and cutlery (for use during quarantine), electric kettle and electric steamer 5) Garbage bags for proper disposal of trash 6) Large can of Sodium Hypochlorite or a disinfectant like Lizol, and hand sanitisers 7) Mobile charger, cable, power bank, laptop 8) Cash, credit card, cheque book, banking details, etc., for payments at the hospital |
How to help contact tracing
It is good practice to keep a journal listing your daily contacts. In case you test positive, all your contacts can be quickly informed and asked to go into quarantine.
If your household help, cook or driver are primary contacts, ensure you/your family members inform them immediately. They as well as their other contacts (secondary contacts) need to quarantine themselves as per BBMP surveillance team’s orders.
Share the name and phone number of your primary contacts in the last seven days, with the government surveillance team . If you had visited public places like shops, office, gatherings, etc., list this down along with the date and time. Keep this list ready to hand over when required.
4. Moving to a COVID Facility
Based on the screening, the patient is recommended one of the following options – home isolation, or treatment and isolation at Covid Care Centres (CCCs), government hospitals or private hospitals.
Asymptomatic Patients
Those with body temperature less than 37.5℃, and SpO2 levels over 95%. They are moved to a Covid Care Centre (CCC) or advised home isolation.
CCCs are hotels, hostels, halls, etc., which have been turned into facilities for COVID patients. Earlier, they were only meant for symptomatic non-patients, but now mild or asymptomatic cases are treated there.
All CCCs are to be equipped with pulse oximeters, handheld thermal scanners, and BP apparatus. They are also supposed to have one nurse per 500 patients at all times.
“Patients are given a choice on how they want to be treated, depending on their symptoms. If the patient’s symptoms are minor, as is likely to be in most cases, they are given the choice of either isolating at home or at a COVID Care Centre. We expect that most will choose home isolation when possible, as the important thing is to save beds for those who really need it [severe patients],” says Dr Giridhara.
Home Isolation for Asymptomatic Patients To be eligible for home isolation, you must meet the following criteria: * Assessed by the health team of district/BBMP authorities * Has to be clinically asymptomatic/mild: temperature <38℃, SpO2 levels > 95%, age below 60 years * Should not have co-morbidities such as kidney disease (requiring dialysis), heart disease, stroke, TB, cancer, HIV. Should not be immuno-compromised, or be on steroids or immunosuppressants * Pregnant women four weeks before the expected date of delivery are not eligible for home isolation * Must have necessary facilities for self-isolation at home and quarantining of immediate contacts - separate and well-ventilated room * If the home is not found to be suitable, or if the patient’s symptoms worsen, they are moved to either CCCs or hospitals. Read full guidelines on home isolation here (Karnataka government's Covid-19 site).
Symptomatic Patients
“If the medical team finds that you have symptoms which require treatment, there are three options – government COVID hospitals (free treatment), private hospitals (with insurance), and private hospitals for those who can pay more for treatment,” says Dr Giridhara.
According to a list released on July 4 by Dr Sudhakar K, Minister of Medical Education, there are 19 government hospitals/medical colleges for COVID treatment in Bengaluru. Of these three are Designated COVID Hospitals (DCHs) and 16 are Designated COVID Healthcare Centres (DCHCs).
There are 72 private hospitals for COVID treatment in the city, according to Dr Sudhakar, Minister for Medical Education.
There are two ways to get treated in private hospitals. If a patient is referred to private institutions by public health authorities, treatment cost is subsidised by insurance packages under the Ayushman Bharat-Arogya Karnataka (Ab-Ark) scheme.
Cost is higher if a patient approaches private hospitals directly, though the state government has capped costs. Following is the per-day treatment cost fixed for private hospitals.
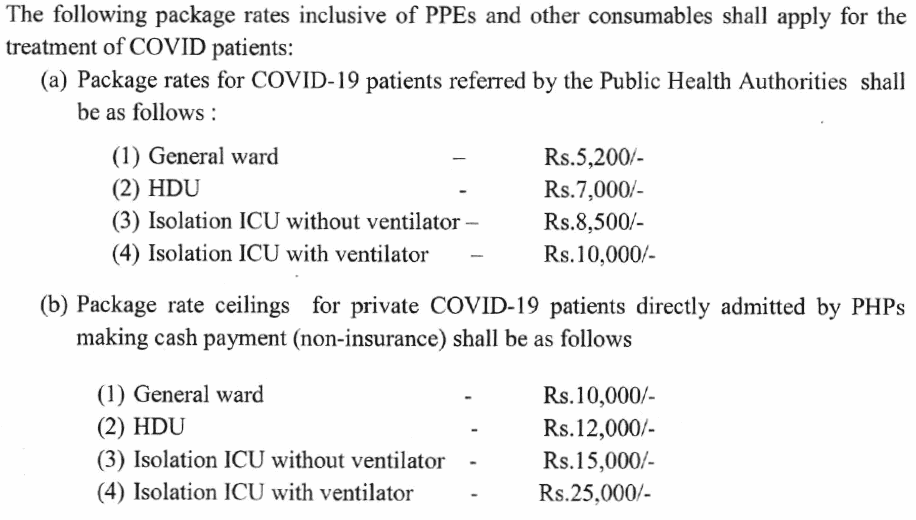

Whether you are sent to a DCHC or DCH will depend on your symptoms.
- Patients with mild-moderate symptoms
If body temperature is more than 37.5℃ and SpO2 levels are between 90-94%, the patient will be moved to a Dedicated COVID Healthcare Centre (DCHC).
At the DCHC, a more comprehensive health check-up will be done. Your BP, temperature, oxygen levels, blood sugar levels, renal and liver function tests, CBC, ECG, etc., will be checked. Depending on your results, you may be sent to a Dedicated COVID Hospital (DCH) for more comprehensive treatment.
- Severe Cases
If your oxygen levels are below 90%, you will be sent to a DCH directly. If you’re aged above 60 years with comorbid conditions or are immuno-compromised, the same applies. If a patient’s health deteriorates at a CCC or DCHC, they too are sent to a DCH.
- Dial 108 for Arogya Kavacha ambulance to shift patients
- Dial 1912 if a government or private hospital denies bed
108 service will ascertain if the person is COVID-positive or a suspected case, and arrange for an Advanced Life Support (ALS) ambulance to a nearby treatment facility in consultation with the BBMP’s bed allocation team.
If the person has not undergone a COVID-19 test, but has breathlessness, asthma or ILI, they will be shifted immediately to a COVID hospital and tested compulsorily.
5. Discharge
After treatment, a patient can only be discharged if they meet certain criteria. All discharged patients are to be under 14 days of home quarantine and self-monitoring.
Following are the discharge criteria for different categories of patients:
Asymptomatic
- No symptoms
- No fever
- Oxygen levels over 95% maintained
- Respiratory rate less than 24 per minute
- Patient remains asymptomatic 10 days after the test
Mild/moderate symptoms
- No fever or symptoms for three consecutive days
- 95% oxygen levels for four days
- Resolution of breathlessness and inflammatory markers
- Above conditions are maintained for at least consecutive 10 days after onset of symptoms
Severe symptoms
- No fever or symptoms for three days
- Oxygen at 95% for four days
- Resolution of breathlessness and inflammatory markers
- Complete clinical recovery
- Should test negative three days after recovery
[Corrigendum: This article previously said that pregnant women four weeks before the expected date of delivery are eligible for home isolation. This has been corrected to say that this category is not eligible for home isolation.]
Also read
► Eight things you must know about insurance policies covering COVID-19 treatment
► What to expect and how to cope if you test COVID positive in Delhi
Thanks
Thank you for a detailed article
Thank you for the details
Very informative and simple to understand. Thank you so much
Wow, this article has really detailed everything. Thanks for publishing.
Hi iam raji from Shri Padmashree High School, bangalore. Thank u for the detailed information.
I will share this link with my students and parents.
There few more things need to known….?
very good information
Thanks. Very informative.
Your article is too good. The information provided is too relevant and is very helpful for every individual … Good work. STAY HOME STAY SAFE AND STAY HEALTHY…
I am bookmarking this page. Thanks for such a comprehensive information.
The package rate is for one day or for whole treatment tenure of 14 days
Mostly per day.
Hi Ms Kusuma,
This is the per-day rate at private hospitals.
– Ed
Good article information
This was beautifully done. Thank you for taking the time. You have no idea how much better it makes us feel to not be uncertain about what to do and how if ever we are affected by the virus. It’s a huge relief to see it all put down so systematically.
This article has given clear insight of the total process and of the treatment, and contact info.
Very helpful. Thank you
Good information.pl keep updating
Excellent the complete information has been provided and the person should not panic and should follow the guidelines. I am a resident of Hyderabad but still it is very informative. Thanks
Thank you. Very nice article and very informative
Very informative and useful to the major cities.great initiative by the govt and Vivid task force.
Any person should not watch kannada news channels. Watched person’s recovery will be either delayed or he may die also.
Accurately put across for quick understanding. Thank you sir.
What happens to the children if both parents are shifted to covid facility
V.good detailed info at one place.
Thank you so much for the govt in release this article hope everybody follows this with no loop holes
Very informative
Thanks very helpful
Thanks siddhant. Very informative and helpful.
Thanks for posting such a highly informative article. This is the best on Corona, so far. Thanks again!!
Good information
Very nice article and clear information about present challenging environment
Very nice information
Comprehensive article.
Primary and secondary family members should get tested even after affected person is asymptomatic for 15 days from passitive date of result and home quarantined, No symptomatic for family persons?
This is such an illuminating article that lends great clarity in dispelling COVID19 related ambiguities. Your arduous efforts in compiling all the required information in one article are indeed commendable! appreciations and well done.
Full information on the decease & how to face the situation in case of necessities, who are the authority to contact. Very useful & handy IN ONE PLACE
Very informative, thanks and God bless
Thank you for the first clear, non contradictory guideline on Covid 19.
Informative…. Tq..
This is really a great article with clear detailed information
Very good article, exactly what every one was looking for
Very nice and informative very useful for all the citizens
Thanks alot for precautions, more information clearly explained , all here with out missed any , no doubts on this covid to ask anyone
very informative. Thank you.
Thank you so much for the details,
Firstly, I want to thanks to those people who have come in forward to take a stand and fight against the coronavirus during these difficult times, Shame on those people who have said bad about Bangalore coronavirus peak cases?I being a locality of Bangalore wanted to tell that it all started spreading from the outsiders who are working in Bangalore otherwise, Bangalore likely to be a safer city In all the ways.
Very very good information.
Thanks to informers.
Sidhant, very well written, systematic, easy to read and understand. Thank you. Is it possible to take a printout.
Useful article with end-to-end information.
Please convert this into a booklet for quick reference. This could be subsidized by voluntary sponsors. Though booklet won’t have links, it will be a handy guide.
Very useful information. Could you please provide & recommend the list of few most accurate and reliable brands of Oximeters (both Indian & Imported models) available in India
Thanks for lovely and accurate information. Almighty bless you
Comprehensive details. Thank you
Thanks,,,,,
I along with my son (6 years old) had been found Corona positive on the test done on 29/06/2020 . As per that I was asked to get admitted to the hospital and we both are presently admitted at victoria hospital.
Now it is that, till date my family members been not tested for it.
they don’t have permission to go outside,
they are not getting proper care from government side.
my wife is and brother is working in private firms..
It is that we all need to immediately get clarified with proper test reports to convince our respective offices, so that they can take appropriate action in this regard.
Moreover, my father is a cancer patient ,along with he have seizure disorder, tracheostomy and other problems.
who is also expected to have got infected. In his case a proper backup is required, as there are good chances of this health geting worse.
And my wife 33 week pregnant
Considering the above stated facts, it is requested to please tested my family members immedietly.
Expecting swift action in this regard.
Toms
Mobile no. 9449915511
Address:#301
12th cross
annasadrapalya
HAL 2nd stage.
banglore 560017
https://m.facebook.com/story.php?story_fbid=10220344338771497&id=1020494251
Excellent article..provides detailed information which was hard to find anywhere else..great relief..thanks a lot for writing this…please keep posting updates on this topic..Thanks..
Nice compilation and presentation of what one needs to know and take care of himself or herself and contribute to good community living.
However there is a world of difference in reality even to get the Test done, get result.
It is almost impossible to get admission in good Pvt hospitals (from among those identified).
What a Citizen poor-middle class- affording type needs is contacting one source over phone and that agency must “manage” and “arrange” everything in quick time. Payment / non payment can be sorted out based on categorisation. On one hand we hear only 20 % occupancy and on the other hand I know personally of cases where “patients” had to move heaven and earth. This, for a dreaded Virus. If only we can rectify the deficiencies it would be wonderful.
Information elaborately explained. But actual situation as understood thro mefia is totally different whether any helpline wl respond and ch one yo the rescue of needy That shd b improved and everyone who has symtoms shd get treatment
Very comprehensive. Many thanks for this compilation. Bookmarked the page and have circulated the link also in Whatsapp group.
Detailed and very useful information to all at this critical juncture.
During times of such ambiguity about COVID-19 detection & treatment around the world, this article provides such clear information to the general public.
Kudos to you Siddhant for putting together this piece. And thank you so much!
Useful information. I have been tested positive and I have been recommended for Home Isolation. How come we don’t get the COVID Test results? The test happened at a private lab at my cost. Is there a rule for not disclosing it?
No you will get a report
Great job, extremely informative. Siddhant Kalra, much appreciated.
Thank you for giving a comprehensive explanation.I’ve a couple of doubts:
1. What about patients with insurance?
2. What if no body picks the call?
3. What if a hospital refuses to admit?
4. Whom to contact first in case of doubt of being infected?
Thank you
When can a asymptotic covid patient should be tested again for covid test?
Thank you for this article – how do we keep ourselves updated basis of government rule changes regarding pandemic
If all the members are home quarantined then no need ,I think because ,testing all people again cost is more and poor people cannot bare it,,
Very nice information.
Thanks it was helpful
Primary and secondary family members should get tested even after affected person is asymptomatic for 15 days from date of discharge from the hospital and home quarantined, No symptomatic for family persons?
Again Testing is required for corona patients ?