The leather tanning industry employs 4.42 million workers in India and accounts for 13% of global leather production. However, the dark side of this industry is that leatherwork exposes its workers to several chemicals, most of which are carcinogenic or have substances that can cause cancer.
Research reports the increase in risks for a number of cancers among tannery workers, highlighting their occupational exposure and the allied vulnerability. The tannery workers in Bengaluru are aware of the hazards. C Pasha, who collects skins or hides for the curing units, was quoted in an article saying “people in this work die easily, they get cancer.”
Occupation or profession is an integral part of one’s lifestyle, which means there is a chance that occupation-based risks exacerbate cancer risks. Given India’s largely informal workforce, there is a gap in research that addresses the impact of occupational risks and hazards on workers. Further, existing research says the “estimation of the burden of cancers attributable to occupational exposures is also made difficult by the fact that occupational cancers are usually clinically indistinguishable from those unrelated to occupation.”
But how does one’s occupation or profession impact the likeliness to develop cancer?
What is occupational cancer?
The Indian Council of Medical Research (ICMR) in its bi-annual report highlighted that the national average for the number of cancer cases in 2022 was 100.4 per every one lakh people.
An International Labour Organisation’s study on the prevention and control of occupational cancer defines occupational carcinogens as chemical substances, physical agents or work processes, which may cause cancer due to conditions of exposure in the workplace.

Research that analysed the burden of occupational cancers in developing countries found that “workplaces continue to be a substantial source of carcinogen exposures” and that these environments are more relevant in developing countries, where cancer mortality is increasing.
In a response to Citizen Matters, the office of Dr Prashant Mathur, Director of the National Centre for Disease Informatics and Research (NCDIR), mentions some cancers are closely associated with occupation. These cancers are mainly mesothelioma, lung cancers, bladder cancers and leukaemias (blood cancers). There are many more causes of the mentioned cancers but occupation is one of them.
“Occupational cancer is the possibility of one’s workplace exposing them to some kind of carcinogens (cancer-causing substances), which will lead to cancer,” says Prashant Kesharvani, from Azim Premji University’s School of Development. However, he cautions against equating exposure to the occurrence or a guaranteed diagnosis of cancer.
Workers in Bengaluru
The National Cancer Registry Programme (NCRP) collects data for all anatomical sites of cancer occurring in a defined geographic area, the response from NCDIR added. There is a Population-Based Cancer Registry covering the Bengaluru urban agglomeration since 1981. NCDIR-NCRP collects data on newly occurring cases (incidence) of cancers for all types of cancers (including those associated with occupation).
As per the NCDIR 2012-14 data, the highest cancer incidence was among females between the ages of 55-59 years, with 2179 of them being diagnosed in Bengaluru. 1909 men between the age bracket of 65-69 years had the highest incidence. In total, 13,221 males and 15,828 females in the city were diagnosed with cancer.
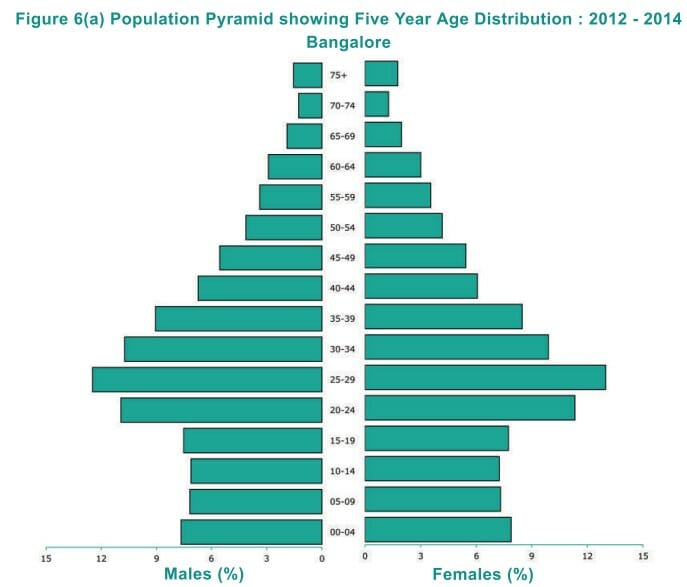
“While Bengaluru has witnessed an increase in incidence, it is still lesser than regions in the north and north-eastern part of India,” Prashant says. What has been seen in the city, especially among males, is that lung-related cancer cases have gone up. This can be related to either an increase in tobacco consumption or air pollution. “Though the Air Quality Index of the city is much lower compared to other northern cities, or for instance, Delhi,” he says.
However, Prashant says that the Registry data is not disaggregated by profession or other socio-economic determinants, except for gender, age, types of cancer and rates of incidence. “So if there is a trend of occupational cancer among a certain social group, we do not have data to track it,” he points out.
The aforementioned paper also notes the unavailability of studies on occupational cancers focusing on the type of employment, which can help identify precarious employment conditions or informal jobs
Read more: E-shram report card: Workers complain of lack of information and interest from city agencies
How do informal workers fare?
There is not a lot of information on informal workers per se, despite them making up 90% of India’s working population contends Abha Rao, research scientist and assistant professor at the Ramalingaswami Centre on Equity and Social Determinants of Health, Public Health Foundation of India. “We know that the construction industry, for instance, in urban India is largely comprised of migrant workers or informal labourers. The construction industry has the highest burden of occupational cancers, this is true globally,” she states, adding that this is because they are exposed to materials such as asbestos and silica.
As Prashant earlier mentions, the development of the disease requires repeated exposure or exposure over time. “An example of this concerns those engaged in dismantling of ships where the workers are exposed to asbestos- a known carcinogen,” Prashant says, adding that repeated exposure could heighten the risk of cancer. Another example of an occupational hazard is exposure to silica. “The workers engaged in mining in certain parts of central India are exposed to silicon which can lead to silicosis and results in breathing problems,” states Prashant. These workers can also be at the risk of lung cancer.
A recent Indiaspend report highlights the long-term exposure of stone quarry workers to silica and deems it an “incurable occupational disease, affecting mostly mine and construction workers.” At 48,448, Rajasthan has the highest number of registered silicosis cases.
Without even counting the people who work in foundries, the tanning industry and other factories where there are exposed to carcinogenic agents, even the workers who work with wood dust are subjected to a higher incidence of lung cancer. “All of this suggests that they (informal workers) probably have a very high rate of occupational cancer, but we just don’t know how high or what rates it is really, ” comments Abha. India’s informal workplaces lack regular inspections and surveys to check if worker protection laws are inspected.
Read more: Migrant workers deal with unhygienic living conditions, poor nutrition
Lack of protection and financial reprieve
Additionally, people in the urban informal sector are also plagued by a multitude of health problems. “Those working in construction are prone to musculoskeletal injuries, due to repetitive motions, and hearing loss due to the noise on construction sites,” Abha says, alluding to the very little physical and social protection that is afforded to the workers.

Referring to her interactions with the construction workers’ community in Bengaluru, Abha mentions that cancer does not play a huge role in the imagination of their health concerns. “A lot of them are very taken by the sort of the day-to-day labour, the musculoskeletal pains, the physical exhaustion, and those kinds of issues play a much bigger role in their lives,” she says. Further, she mentions that they were also worried about workplace injuries.
In terms of the monetary support of reprieve that is available to informal workers, Abha says most of them, especially those working in small construction sites are not unionised, hence they do not get the necessary access to health insurance schemes that comes with union membership. “As far as my understanding goes, there are no specific health programs to address these occupational issues, including cancer, ” she states.
“As per the data, out-of-pocket expenditures on health in India are high compared to other countries. India has one of the lowest expenditures on health by the state, so when the state doesn’t spend, one will have to pay from their pocket. This is also because private healthcare is not regulated, ” says Prashant. While this affects all sections of society, of course, the poor are going to bear a disproportionate burden. This, according to him, means that they will either not avail of services or they will be entrapped in debt, borrow loans or mortgage assets to meet the medical expenses.